 -
- A study of 50 migraineurs has confirmed
previous observations that sleep is a common way
of ending the headache phase. 14 subjects could
shorten attacks by going to sleep during the day
for an average of 2 1/2 hours. Different methods
used by patients to aid falling asleep are
described. 47 of the 50 subjects had symptoms
after the headache had gone--here called the
recovery phase which can double the length of
individual attacks. It is suggested that
prodromata, some symptoms of the headache and
recovery phases, as well as the therapeutic
effect of sleep, indicate that migraine is
primarily a neurological rather than a vascular
disorder
-
- This inquiry was stimulated by a patient
saying that she could shorten and end her
migraine attacks by making herself sleep for two
hours. Perhaps other patients had found similar
or alternative methods to abbreviate attacks
that could be more widely used in treatment.
Furthermore, techniques which resolve migraine
episodes could illuminate the underlying, still
unknown "migraine process" that initiates and
maintains individual attacks.
-
- When asking patients how their attacks
ended, a range of symptoms that persisted after
the headache had resolved became apparent.
Although patients often state that after an
attack they feel "washed out", these symptoms
have gained scant attention, even by Liveing,'
one of the few who annotated how attacks
terminated in individual patients.
-
- Patients and methods
-
- 50 subjects with uncomplicated migraine were
questioned: 29 were patients referred by their
personal physician to a neurological or migraine
clinic; 21 were colleagues and friends, 11 being
medically qualified. Having ascertained that
they had migraine as previously defined ,2 each
was asked how their migraine ended and if they
had tried or found ways of shortening attacks,
then how they felt after the headache had gone,
followed by specific questions about feeling
tired, yawning, mental, physical, alimentary and
urinary symptoms, and their duration. The
answers to questions about the same symptoms
before and during the headache phase were also
sought and recorded. Ages ranged from 21 to 64
years with an average of 42 years. 35 were
female and 15 male. 34 had prodromes3 and 16 a
classical aura.
-
- Results
-
- HOW HEADACHES RESOLVED
-
- Slowly during the day: 18 subjects found
that their headache decreased imperceptibly
during the day"it just drifts away", or "I
realised it had disappeared during the morning
or afternoon". Rapidly by day: eight individuals
noted a rapid decline of pain estimated between
and 1 hour; in four of these, vomiting preceded
pain relief. Sleep at night: 28 of the 50
subjects noted relief from headache after a
night's rest. Many retired early if the pain was
moderate or severe, if it was opportune to do
so. A few added that such a sleep seemed
particularly deep. Sleep by day: 14 subjects
ended some attacks by going to bed during
daylight hours, always excluding light by
drawing the curtains or putting the head under
the bed clothes. Additional methods to attain
sleep will be detailed in the next section. The
duration of day-time sleep required to end the
headache varied from to 6 hours, the average
being 2,5 hours. One physician found that "a
siesta of hour sufficed". Another consultant
physician, if his headache was severe while at
hospital, would sit and snooze for 10-15 minutes
in a dark quiet place until his pain diminished
sufficiently to complete the day's work and then
go home, early to bed. Of the 50 subjects, 29
felt that one of the above modes predominantly
ended attacks, 19 by two methods, one by three
and one in four different ways. A few observed
that the pattern of ending attacks changed as
they grew older, but all agreed that no method
was invariably efficacious.
-
- METHODS OF ABBREVIATING OR REDUCING SEVERITY
OF ATTACKS
-
- 18 subjects said that nothing helped to
shorten attacks which had to take their own
course. This did not inhibit patients taking
analgesics, anti-migraine preparations or
retiring earlier than usual to try and end their
attacks. Of the remaining 32, the following
methods (table) at times, but by no means
invariably, reduced the length or the severity
of attacks, or both. Some subjects used a number
of techniques.
-
- A number of subjects talked about trying to
go to sleep. One "switched off mentally", and
another "reduced the work load" implicating a
conscious effort to relax or go to sleep but
they could not specify how they achieved their
result.
-
- SYMPTOMS AFTER HEADACHE HAD
DISAPPEARED-RECOVERY PHASE
-
- Only three patients in this series were
totally symptom-free once the headache ceased.
The other 47 had mood variations, muscular
weakness, abnormal appetite, yawning, tiredness
and changes in fluid balance. 31 of these 47 had
multiple symptoms: "tired and washed out" was a
common expression, for feeling mentally and
physically below normal. Although the symptoms
lasted from 1 hour to 4 days in individuals,
"the rest of the day", "the following morning"
or "the whole of the next day" were usual
descriptions. All patients commented that the
post-headache symptoms were more marked after
moderate or severe attacks.
-
- MOOD CHANGES
-
- Elevation of mood from slightly euphoric to
"on top of the world with a desire to
spring-clean the house" or "high and really
happy" occurred in eight. More frequent, in 28,
was a lowering or mood and intellect,
interfering with figure work, concentrating,
alertness, unproductive (a research scientist),
inclined to finish the morning clinic at 11.30
am instead of 1 pm (a consultant physician),
dopey, irritable, low, lifeless (a journalist),
muddled, inattentive, sluggish, not fully alert
and distant were terms used. In most instances
routine work was possible but more arduous or
creative mental activities were difficult, or
not tackled.
-
- PHYSICAL AND MUSCULAR SYMPTOMS
-
- Physical tiredness featured in 26 and
muscular weakness in 27. In extreme instances
aching muscles were compared with an influenzal
illness. Others lacked normal energy-"just get
meals but not a lot of housework" (a 35-year-old
housewife), or "ordinary daily activities but
not playing football or badminton" (a
26-year-old bank official).
-
- APPETITE AND FLUID BALANCE
-
- Restricted food intake was noted by 16
subjects, especially intolerance to rich, fatty
or spicy foods. Bland meals that could be taken
included boiled potatoes, steamed fish, a
sandwich and "carbohydrate in general" (a
doctor), toast, biscuits were common. Two
subjects specifically desired dry toast and
Marmite and six expressed a need for sweet foods
or sweets, similar to the cravings experienced
during the prodromal phase.3 Seven passed more
than usual amounts of urine, two less and four
were thirsty.
-
- YAWNING AND TIRED
-
- Four yawned excessively, one without feeling
tired, while in the other three excessive
tiredness was evident.
-
- OTHER FEATURES OF ATTACKS IN THIS
SERIES
-
- Prodromal symptoms occurred in 34 of the 50
patients, many having more than one symptom.
Attacks were heralded by mood elevation (13),
depression (12), yawning (15), undue tiredness
(10), anorexia or nausea (6), constipation (3),
loose bowel action (2), increased desire for
food, usually sweets or chocolate (8), fluid
retention (3), feeling unduly cold (2), sneezing
(1) and sweating (2).
-
- The duration of prodromal symptoms before an
aura, if one occurred, or before the onset of
headache ranged from I to 48 hours: the average
in 34 subjects was 12 hours. The high incidence
of prodromes may be due to including some
subjects from a previous series.3
-
- Aura 16 patients had an aura, visual
disturbances for 15-30 minutes (12),
dysaesthesiae or dysphasia for -2 hours (3), or
brain-stem features of basilar migraine lasting
1 hours (1). The average duration in this group
was 40 minutes.
-
- Duration of the headache phase Headaches
lasted from 4 hours to 35 days, the average in
the 50 cases being 21 hours.
-
- Sleep The range of sleep duration during
which the headache disappeared was -6 hours, if
patients slept by day, or 8-12 hours during the
night, depending on whether they retired early
or at the normal time-a mean of 7 hours.
-
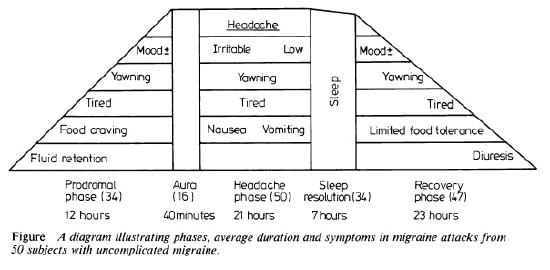
- SUMMATION Of TIMING AND A DIAGRAM
-
- The duration of the various phases is based
on each patient's estimate, liable to be
influenced by the most recent attacks in some,
or recollections of more severe attacks in
others. Hence the times are approximate. 1f a
patient said that a particular phase took 4-6
hours, then 5 hours was taken, or -21-1 day then
18 hours was accepted. On this basis a diagram
(fig) was drawn.
-
- Discussion
-
- The observation that sleep resolved migraine
attacks was recorded 100 years ago by Liveing'
who mentioned a number of his famous
contemporaries whose attacks ended in this way,
including DuBois Reymond, the discoverer of the
electrical nature of the neural impulse. More
recently Dr Marcia Wilkinson has maintained that
an anti-emetic followed by an analgaesic enabled
patients to go to sleep, and it was the process
of sleeping that relieved the headache most
efficiently. She has proven her point by a
statistical analysis of 310 patients treated at
the City Migraine Clinic in London.4
Confirmation comes from a headache clinic in New
York: Coddon (personal communication) gave
intravenous chlorpromazine, diazepam and then
sodium amylobarbitone. He found that 3-4 hours
sleep was essential to end migraine
attacks.
-
- The therapeutic implications for migraineurs
are self-evident: they must become acquainted
with the various known methods of stopping
attacks and experiment on themselves to discover
which method or combination helps them. It could
prove beneficial to those patients whose attacks
resolve during sleep to study how to get to
sleep as soon as possible after the onset of
symptoms, even by day. Darkness, lying down
(although a few prefer to sit), heat or cold,
anti-emetics, analgaesics, anti-migraine
preparations, singly or in combination may
assist falling asleep. Perhaps the
pharmaceutical companies should reconsider the
inclusion of caffeine in their antimigraine
compound preparations, another point made by Dr
Wilkinson and supported by this study.
-
- The theoretical significance of sleep in
relation to migraine needs appraisal. Normal
sleep is thought to have a restorative
function.5 Sleep after a migraine attack could
therefore be a non-specific response to stress,
pain, vomiting or lack of food. Alternatively
somnolence, yawning and sleep may be integral to
the altered physiology in migraine, a notion
supported by these observations: attacks can be
precipitated by lack of sleep, becoming
excessively tired or sleeping too long; yawning
and tiredness are prodromal symptoms that may
continue during, as well as after, the headache
phase.
-
- The sleep-waking cycle is affected by
hypothalamic disturbances. Other cyclical
changes implicating the hypothalamus shown by
the migraineurs in this series were mood
variations, fluid retention, diuresis,
hyperphagia, nausea and vomiting followed by
restricted food tolerance. Hence
neuro-endocrinological studies, particularly of
the hypothalamus suggested by Herberg,6 could be
rewarding. A potential mechanism for these
vegetative symptoms has been postulated
recently.7
-
- Finally, turning to the underlying migraine
pathogenesis is it vascular or neural ?
Discussing this problem, Gowers wrote 100 years
ago, "the vascular system is in a special way
under the influence of the cerebral centres. An
emotional blush and the pallor of fear are
conspicuous examples of this fact. It is at
least as easy to conceive that the vascular
changes are the result of the disturbance in the
sensory centres, or are the effect of associated
derangement of the vasomotor centres, as it is
to consider that the vascular condition is the
primary change".
-
- If Gowers'
analogy is valid, then the vascular changes in
migraine would be secondary to focal cerebral
metabolic or primary neural disturbances. Recent
experimental evidence indicates that vascular
changes follow alterations in brain metabolism.
For example, Sokoloff9 has demonstrated that
functional activity in the central nervous
system regulates local glucose metabolism and
within seconds the regional microcirculation is
secondarily adjusted to the local metabolic
demands.
-
- In migraine research the clinical evidence
must be aramount. The presence of prodromal and
recovery ymptoms suggest that neurological
disturbances form art of the underlying
"migraine process" which still emains elusive.
Although our aim is to abolish the ondition by
prevention, we are not yet in that appy position
and must try to stop attacks as uickly as
possible. Nevertheless, this study supports n
old observation, the importance of sleep, which
y itself indicates that further neurological
research i relation to migraine would be worth
while.
-
-
-
-
- -Blau
JN. Resolution of migraine attacks: sleep
and the recovery phase. J Neurol Neurosurg
Psychiatry. 1982;45(3):223-226
- -Blau JN
Migraine postdromes: symptoms after attacks
Cephalagia 1991;11;(5):229-31
-
-
- Bès A
et al Hypersensibilité dopaminergique
dans la migraine: un test diagnostique ?
La Nouvelle Presse
Médicale1982; 11; 19
- Blau JN
Migraine postdromes: symptoms after attacks
Cephalagia 1991 Nov; 11; 5;
229-31
- Blin O,
Azulay JP, Masson G, Aubrespy G, Serratrice
G Apomorphine-induced yawning in migraine
patients: enhanced responsiveness
Clin Neuropharmacol 1991 Feb;
14; 1; 91-5
- Cerbo R,
Barbanti P, Buzzi MG, Fabbrini G, Brusa L,
Roberti C, Zanette E, Lenzi GL Dopamine
hypersensitivity in migraine: role of the
apomorphine test Clin
Neuropharmacol 1997 Feb; 20; 1; 36-4
- Del
Bene E, M Poggioni Video assessment of
yawning induced by sublingual apomorphine in
migraine Headache 1994; 34; 9;
536-8
- Del
Zompo M Dopamine Hypersensitivity in
Migraine: Role in Apomorphine Syncope
Headache 1995; 35;
222-224
- Del
Zompo M Association between dopamine
receptor genes and migraine without aura in a
Sardinian sample Neurology 1998;
51; 3; 781-6
- Fanciullacci
M, Alessandri M, Del Rosso A Dopamine
involvement in the migraine attack.
Funct Neurol 2000; 15 Suppl
3:171-81
- Heinrichs
L Linking olfaction with nausea and
vomiting of pregnancy, recurrent abortion,
hyperemesis gravidarum, and migraine headache
Headache 2003; 43; 3;
304-5
- Jacome D
Compulsive yawning as migraine premonitory
symptom Cephalalgia 2001 Jun;
21; 5; 623-5
- Jacome D
Primary yawning headache
Cephalalgia 2001 Jul; 21; 6;
697-699
- James
MF,Smith J M et al Cortical spreading
depression and migraine: new insights from
imaging? Trends in Neurosciences
May 2001; vol 24; n 5; p 266-271
- Loder
A What
is the evolutionary advantage of migraine ?
Cephalalgia 2002; 22;
624-632
- Peres
MF et al Hypothalamic involvement in chronic
migraine J Neurol Neurosurg
Psychiatry 2001; 71; 747-751
- Peroutka
SJ Dopamine and migraine
Neurology 1997 Sep; 49; 3;
:650-6
- Pietrobon
D, J Sriessnig Neurobiology of migraine
Nature
Neurosciences Reviews may 2003; vol 4;
n°5; p386-398
- Sabatini
U et al Migraine attacks induced by
subcutaneous apomorphine in two migrainous
parkinsonian patients Clinical
Neuropharmacology1990; 13; 3;
264-267
- Szechtman
H et al Sensitization and Tolerance to
Apomorphine in Men: Yawning, Growth Hormone,
Nausea, and Hyperthermia
Psychiatry Research 1988, 23,
245-255
-
|

