Case report : A 28-year-old
black man was admitted to San Francisco General
Hospital after being knocked out during an
altercation. He was unconscious for an unknown
period of time, but was subsequently taken home,
where he slept for about 10 hours prier to
admission. His initial complaints included
headache, more severe on the left than on the
right, and bloody drainage from the left car. He
denied prior problems with his ears or facial
paralysis.
Physical examination revealed an alert man
with bloody otorrhea on the left. A tender boggy
hematoma was present in the occipital area on
the left, but there was no Battle's sign.
Moderate swelling in the left parotid region was
noted. The mandible deviated to the right on
opening but the mandible and maxilla were
intact. The left tympanic membrane was torn and
a trickle of blood was seen coming from the
middle ear. The Weber lateralized to the left,
and the Rinne test was negative at 512 Hz on the
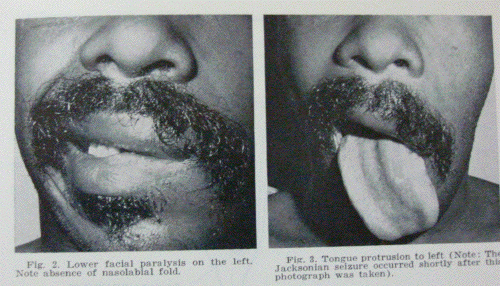
left. A partial left facial paralysis was
present, with inability to close the eye
completely, wrinkle the nose, or smile. There
appeared to be near normal voluntary movement in
the forehead and platysma. The patient's mouth
was noted to be nearly symmetrical at rest. The
tongue deviated slightly to the left on
protrusion. Skull X-rays were negative for
fracture.
A diagnosis of left temporal bone fracture
with facial nerve laceration or contusion was
entertained, but the correct diagnosis became
apparent when the patient laughed at a joke,
exhibiting a normally symmetrical smile. He
then yawned, and the upper and lower lips again
moved symmetrically. Confirmation of the
supranuclear contralateral location of the
injury came when seizure activity was seen
commencing in the left nasolabial fold area, and
marching in true Jacksonian manner to involve
the entire face on the left, masseter and
temporalis muscles, tongue, sternocleidomastoid,
and musculature of the upper arm on the left.
The seizure lasted approxiniately 90 sec and
resolved spontaneously. Postictally, the facial
paralysis persisted to voluntary mimetic
efforts, but emotional movements were normal.
Eye blinking was normal in response to corneal
stimulation, but the patient was unable to
completely close the left eye voluntarily. One
gram of phenytoin was given intravenously, and
no further seizures were noted. The patient
signed out of the hospital before an
electroencephalogram or computed tomographic
brain scan could be done. The patient has not
returned for follow-up examination, but reported
by telephone that the facial paresis resolved
after a few days.
Comment : The paralysis of voluntary
facial motion with retention of involuntary
movement is easily explained by the neuroanatomy
of the facial nucleus and its multiple
supranuclear pathways. Volitional facial
movements originate in the cerebral cortex of
the precentral gyrus, and impulses pass through
fibers in the internal capsule to synapse in the
facial nucleus. The frontalis, corrugator
supercilii and orbicularis oculi muscles are
innervated by a clearly delimited area of the
nucleus, the pars intermedia. The supranuclear
innervation of this part of the nuclelis is both
crossed and uncrossed, e.g., from both right and
left sides of the cortex. This is why most
central paralyses exhibit sparing of the upper
face. (In this regard, May has shown that it is
possible for a temporal bone fracture, or a stab
wound of the parotid gland, to produce a facial
paralysis with sparing of the upper face, due to
the spatial orientation of fibers in the nerve
trunk.) The "pseudo-peripheral" paralysis of the
operculum syndrome does not usually spare the
upper face, although in our patient this was not
the case.
At least six other sites of innervation for
the facial nucleus are known, each of which is
responsible for a particular reflex or specific
muscle stimulation. Fibers from the superior
colliculus are responsible for the blink reflex
in response to a bright light. Connections with
the trigeminal nuclei produce a blink in the
corneal reflex. Emotional smiles invoked by
happiness or humor are the result of innervation
of the facial nucleus by fibers front the
thalamus and the globus pallidus. Tlie
involuntary periodic blinking of both eyes is
due to additional afferents from the reticular
formation and/or basal ganglia. The stapedial
acoustic reflex is mediated produced by fibers
from the nucleus of tractus solitarius.
All of these "lower reflex" movements of
muscles innervated by the facial nerve are
preserved in patients with cortical or high
corticobulbar lesions. Disorders of the
brainstem and/or midbrain, on the other hand,
may cause a paralysis of these reflexes, while
voluntary movements (as the "social" smile) are
preserved. There is evidence that a second
cortical region located in the temporal lobe
participates in the emotional smile pathway. A
reciprocal picture, then, is seen in patients
with lesions of these lower centers, e.g., in
paralysis agitans or postencephalic
Parkinsonism, voluntary or mimetic movements are
normal while emotional facial responses are
lost.