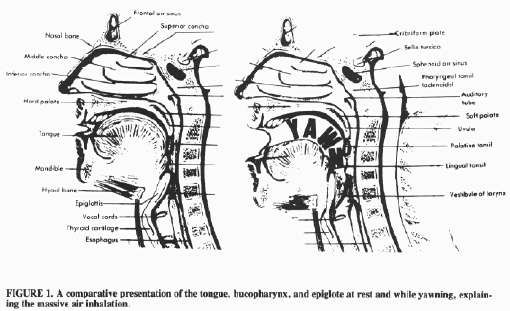
Yawning consists of an involuntary wide
opening of the mouth, with maximal widening of
the jaw, and long and deep air inhalation
through the mouth and nose followed by a slow
expiration. As a result, an increased amount of
air is inspired in the lungs (Figure 1).
The average
duration of the yawn is 5 s, (range, 3 to 45
s).
Yawning may be associated with tears,
shivering, obstruction of the eustachian canal
(causing a reduction in audiologic acuity), or
stretching of the limbs. During monotonous work,
yawning may be preceded by looking about,
changing position, or arranging one's hair.
Female infants yawn more than male infants
(Feldman, Brody, & Miller, 1980), a ratio
that later becomes inversed.
The earliest appearance of yawning was
observed in a
15-week-old embryo (De Vries, Visser, &
Prechtl, 1983). Fetal yawning appears randomly,
in contrast to fetal hiccups, which appear in a
frequent rhythmic pattern (De Vries, Visser,
& Prechtl, 1985). In newborn babies, a yawn
occurs a few minutes after the first breath and
the first oral cues (Gill, White, &
Anderson, 1984). At 2 months of age, babies yawn
when separated from their parents. The frequency
of yawning decreases with maturation, and it may
be speculated that connections between the
limbic system and the forebrain areas are
already established (Fogel, 1980).
Etiology : The causes of yawning, as
described in the medical literature, can be
classified in seven groups (see Table 1).
Boredom is sometimes associated with the yawning
reflex (Bell, 1980). Boredom occurs; when the
main source of stimulation in a person's
environment no longer sustains his or her
attention, by content or by form. At this
moment, the mind has to make an effort to
maintain contact with the environment;
structures involved in this process include the
prefrontal area and the limbic system. Boredom
induces drowsiness by stimulating the sleep
generating system through the interconnection of
the prefrontal area and the limbic system with
the serotoninergic raphe pontine nuclei and the
ascendant activatory reticular system (AARS).
When boredom is associated with fatigue, the
latter potentiates the drowsiness-inducing
effect (Suganami, 1977). Drowsiness is the most
common stimulus of the yawning reflex.
During a yawn, massive inspiration of oxygen
and the exhalation of C02 serve to reverse blood
hypoxia and to increase the metabolic rate. The
inhalation stretches the bronchial musculature,
stimulating the vagal terminals and the
cholinergic pathway, which dilate arterioles,
thus lowering peripheral circulation resistance
and enhancing blood flow (Friedell, 1974;
Lehmann, 1979; Twiest, 1974). Gaping jaws and
stretched limbs have important circulatory
effects. The lateral pterygoids and the soleus
muscle contain rich venous plexi within their
mass, which empty with the contraction and are
therefore called "peripheral hearts." Through
this mechanism, venous return is enhanced
(Bhangoo, 1974; Last, 1963; Siegal, 1974). The
diaphragm contraction associated with the deep
inspirium also enhances venous return, reviving
circulation. The hyperoxygenation and increased
blood circulation stimulate all the cephalic
structures, including the AARS (Montagu,
1962). Monitoring jugular 02 partial pressure,
cerebral blood flow, and electroencephalograms
(EEGs) in thrombotic patients, Karasawa et al.,
(1982) found that yawning appeared when the EEG
showed slow frequency and the oxygen monitoring
showed decreased O2 partial pressure. Thus,
boredom, drowsiness, and fatigue lead to
hypoxia, reduced metabolic rate, and increased
secretion of hypnogenic derivatives. Yawning is
the reflex answer of the AARS, whose aim is to
reverse drowsiness, maintaining the brain at the
level of alertness needed for wakeful
activities.
It may be hypothesized that the yawning
center is a complex neuronal reflex system,
located at the level of the reticular brain stem
close to the AARS. The reticular neuronal
yawning complex is intimately interconnected
with (a) the three aggregates of respiratory
neurons located in the medulla, dorsal, ventral,
and parabrachialis; (b) the motor nuclei of the
fifth, seventh, ninth, tenth, and twelfth
cranial nerves; (c) the phrenic nerve; (d) the
motor roots of the intercostal nerves; and (e)
the parasympathetic terminals of the lacrimal
gland.
The yawning neuronal complex enables
concomitant massive inspiration, with opening of
the mouth accomplished by the digastric and
milohyoid muscles and retraction of the jaw
achieved by the posterior fibers of the temporal
muscles and the geniohyoid muscles. Yawning
sometimes provokes a mass response in which
stretching of the four limbs appears together
with tears or shivering (Bhangoo, 1974). The
following arguments can be presented in favor of
the location of the yawning neuronal complex in
the brainstem reticular system close to the
AARS. A tetraplegic patient with a Pontine
glioma was able to yawn despite the fact that he
could not open his mouth at will (Geschwend,
1977). Opening the mouth through a motor cortex
command was impossible, but reflexogen yawning
was still possible because of the short
interconnections between the reticular neurons
and the motor axons of the fifth and seventh
cranial nerves.
Another tetraplegie and "locked-in"
syndrome patient, suffering from an anterior
pons glioma, could yawn but couldn't open his
mouth at will (Bauer, Gerstenbrand, & Hengl,
1980). The preservation of the reticular complex
center and of the AARS in this patient made
yawning possible. Yawning in a schizophrenic
patient was observed to be related to increased
vigilance (Beckmann & Zimmer, 1981). Yawning
persists in the vegetative state with
spontaneous breathing. In these patients, the
reticular system and AARS are preserved
(Braunwald et al., 1987). Jurko
and Andy (1982) suggested that the
persistence of yawning following thalamotomy is
due to the preservation of the hindbrainstern
reticular system.
Pimozide, a neuroleptic, abolished
valproate-induced yawning through its inhibitory
effect on the AARS (Rollinson & Gilligan,
1979). Bombardment of the AARS by transcutaneous
application of a high frequency electric current
of 300 mA for 30 min decreased yawning
significantly in 11 heroin addicts aged 18 to 31
by slowing down the threshold of the defense
reflex (Daulouede, 1980).
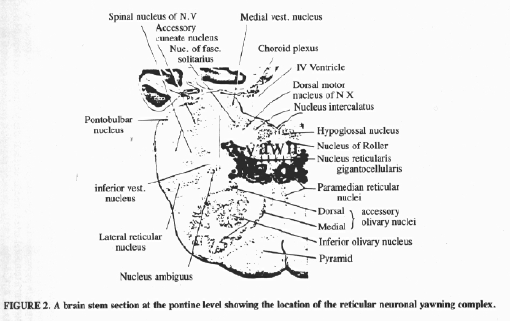
The yawning
reticular neuronal complex bas close
connections with a large number of subcortical
and cortical structures (Figure 2). The link
with the hypothalamo-hypophysary formation is
suggested by the capacity of ACTH and MSH (see
Table 1) to provoke yawning and by the
sensitivity of this area to sleep-promoting
factors and drowsiness-inducing states. The
specificity of boredom as a stimulus of yawning
shows the close interrelationship between the
limbic system and the brain stem areas. A
conversation or a bad movie or book are potent
yawn releasing stimuli, showing the role of the
cortex, especially the occipital and associative
areas. Auditory perceptions of a monotonous
voice, music, and periodic noise are potent yawn
releasing stimuli, showing temporal area
involvement in yawning. Thinking about yawning
is a potent stimulus, which reaches the motor
cortex through the prefrontal associative area
and affects the brain stem yawning center, thus
provoking the reflex (Provine
& Hamemik, 1986; Small, 1977). The
infectiousness of yawning among subjects who are
not bored, drowsy, or fatigued proves the
existence of efférent connections between
the motor cortex and the brain stem reticular
center.
The
Biochemistry of Yawning: Yawning was
suppressed by the opiate antagonist naloxone but
was provoked by administration of naloxone in
drug addicted patients and in normal cigarette
smokers (Flechter, Cohen, Borenstein, Regev,
& Vardi, 1982; NemethCoslett &
Griffiths, 1986; Paroli, Nencini, &
Moscucci, 1984). The hypothalamic peptides ACTH
and MSH, given intracranially, induced a
peculiar stretching and yawning syndrome
associated with penile erection and ejaculation
(Donovan, 1978). Despite the fact that the
intimate mechanism, of the endorphines in
yawning remains unknown, there are several
empirical observations of endorphine involvement
in the yawning reflex (Donovan, 1978; Fletcher
et al., 1982; Nemeth-Coslett & Griffiths,
1986; Paroli et al., 1984).
Pimozide, a haloperidol-like dopaminergic
antagonist, abolished valproate-induced yawning
(Rollinson & Gilligan, 1979). This
observation, together with die observation that
individuals suffering from, Parkinson's disease
yawn less, suggests that dopaminergic receptors
may be involved in the complex yawning
reflex.
Experiments on rats have shown that increased
serotoninergic activity induces yawning
(Holmgren, Urba-Holmgren, & Rodriguez,
1980). Bombardment with hypnagogic derivatives
of the pontine serotoninergic raphe nuclei
induces yawning before the onset of sleep.
Serotonin is considered to be a positive
modulator of the cholinergic activity that sets
off the yawning reflex (Holmgren et al.).
Serotoninergic-induced. yawning increases
cholinergic activity, and through an inhibitory
feedback mechanism, decreases serotoninergic
activity. As long as yawning continues, sleep
initiation is avoided (Friedell, 1974; Lehmann,
1979; Twiest, 1974). The end of yawning is
associated with a feeling of comfort, the result
of a temporary victory over the onset of
sleep.
A certain constellation of neurotransmitters
may favor the yawning reflex. This constellation
includes increased serotoninergic activity and
changed cholinergic, peptidergic, and
dopaminergic receptor activity. This pattern
suggests that yawning has an antisleep
effect.
The
Pathology of Yawning: Yawning may occur
not only because of boredom, drowsiness, or
fatigue but also in association with various
pathologies. For example. psychoneurotic
patients can present a state of repetitive
yawning with a rhythmic periodicity lasting for
9 to 12 min. The rate of yawning is usually 2 to
4 yawns per min (personal observation; Marcus,
1973).
- The Fatal Yawn : When boredom,
fatigue, and drowsiness overcome a driver during
a long and fast journey, a noisy yawn may be a
sign of imminent sleep and, possibly, a fatal
road accident. Nakanishi, Hinoki, Ito,
Izumikawa, & Baron (1980) found this fatal
yawn to be related to an autonomic nervous
system disturbance. The fatal yawn must be
differentiated, however, from car-sickness
yawning, which appears in scoliotic females and
is associated with nausea and vertigo during
driving.
- Recurrent Cerebral Ischemic Yawning :
Yawning was responsible for transient ischemic
attacks in a patient who underwent a temporal
artery-middle cerebral artery bypass operation
(Handa, Nakasu, & Kidooka, 1983). Yawning
provoked recurrent cerebral ischemia by kinking
the donor artery with each wide mouth opening.
Yawning associated with a slow EEG due to
borderline hypoxia was present in occlusive
cerebrovascular patients (Karasawa et al.,
1982).
- Synkinetic Yawning : Mulley (1982)
found yawning with synkinetic movements in the
hemiplegic arm in 80% of 40 hemiplegic patients.
Much less frequent synkinesias were observed
during stretching, coughing, and laughing.
Voluntary movements diminish synkinesias.
Sinkinetic yawning indicates poor prognosis for
hemiplegics (Mulley).
- Yawning Epilepsy : Yawning associated
with head extension and occipital headaches
showed general dysrhythmic activity on the EEG
record of a 35-year-old woman, who was diagnosed
as having diencephalic epilepsy. The
administration of naloxone hydrochloride
suppressed the attacks, suggesting disturbed
endorphine receptor activity (Flechter
et al., 1982). This case resembles the patient
described by Jacome, McLain, and Fitzgerald
(1980) whose volitional head and neck extension
precipitated laughing epilepsy associated with
orgasmolepsy. Ratner and Kaisarova (1981)
observed 12 children in whom a prolonged
inclined position of the head or prolonged
stress provoked yawning, headache, and neck
pain, followed by unconsciousness lasting 20 to
30 min. The unconsciousness was followed by
several hours of muscle atonia. Ratner and
Kaisarova named these attacks "syncopal
vertebral syndrome."
- Yawning and Orgasm : Yawning
associated with orgasm appeared as a side effect
of clomiprarnine treatment in a depressed
patient and disappeared when treatment ceased
(McLean,
Forsythe, & Kapkin, 1983).
- Drug Withdrawal : One of the most
frequently encountered pathologic associations
of yawning is withdrawal from opiates. Yawning
associated with sneezing, profuse sweating, and
vomiting in infants 2 to 3 days old is a
withdrawal reaction to maternal. heroin,
morphine, or methadone addiction (Rudolph,
Barnett, & Einhorn, 1977). In a
lefetamine-addicted adult, who was using this
opiate drug at a dose of 0.9 to 1.8 g/day, the
withdrawal syndrome appeared when 140 mg of
naloxone per day was administered. The syndrome
consisted of yawning accompanied by a
sympathicornimetic reaction of midriasis,
piloerection, and arterial hypertension (Paroli
et al., 1984). Among heroin addicts, withdrawal
consists of yawning, profuse sweating, digestive
disorders, and agitation (Daulouede, 1980). A
withdrawal reaction to pentazocin, a
morphine-nalorphine-like narcotic, consists of
prominent yawning associated with general
epileptic seizures. Greater drowsiness and
respiratory depression différentiate the
effects of pentazocin from those of morphine,
and consequently the defense arousal reaction to
borderline hypoxia resulting from pentazocin's
withdrawal is made more active (Krupp &
Chatton, 1977). Withdrawal from methadone
consists of yawning accompanied by lacrimation,
rhinorrhea, coughing, gooseflesh, tremor, hot
and cold flashes, abdominal cramps, muscle
aches, nausea, vomiting, and diarrhea (Lett,
Wilson, & Gambrell, 1976). Naloxone (0.2
mg/kg) provokes yawning in opiateaddicted adults
(Paroli et al., 1984; Nemeth-Coslett &
Griffiths, 1986).
The Psychoanalysis of Yawning :
Boredom lowers concentration capacity, which
stimulates yawning (Suganami, 1977). Sartre,
whose work Nausea was analyzed by Bell (1980)
suggested that boredom and yawning are
associated with existence and being, and not
with freedom and transcendence. According to
Sartre, yawning plays a role in the ethics of
authenticity. Bell induced yawning in
undergraduate subjects by instructing them to
think about it, showing that yawning is a
stereotyped action pattern. A nonverbal
stereotyped pattern may be encountered as
passive violent behavior, expressing refusal to
participate in dialogue.
Prognostic Aspects : Clicks or
crepitations or myofacial pain during yawning
may indicate a temporomandibular
joint disturbance requiring X-ray examination
(Heloe & Heloe, 1979). Yawning in drivers is
a dangerous sign, showing the need for an
immediate stop and rest prior to the resumption
of driving. Yawning is such a stable feature in
withdrawal that it could be used as an objective
component of a conditioned abstinence response
prior to its spontaneous appearance (O'Brien,
O'Brien, Mintz, & Brady, 1975). Yawning
associated with synkinesias in hemiplegics
indicates poor prognosis (Mulley, 1982). In
early schizophrenia, yawning indicates good
prognosis, but in chronic schizophrenia it
indicates poor prognosis (Lehmann,
1979). During coma, yawning predicts the
approach of wakefulness (Braunwald et al.,
1987).
Yawning is a sui generis neuropsychological
field of inquiry, till now neglected by
medicine. I hope that, by delineating this
phenomenon, I have stimulated interest in
further scientific research on this
topic.
- Yawning
and the reticular
formation
Jean Askenasy and Enosh
Askenasy
- References
- Arai, K., Kita, K., Komiyama, A., Saeki, N.,
& Nagao, K. 1. (1986). Progressive
dysautonomia in hemangioblastoma of the fourth
ventricle region. Brain-Nerve, 38, 195-200.
- Ase, Y, Arai, T., Iida, R., & Okada, S.
(1985). Positive middle ear pressure on
tympanogram in sleeping children. Audiology
Japan, 28, 772-777.
- Bauer, G.,
Gerstenbrand, F., & Hengl, W. (1980).
Involuntary motor phenomena in the locked-in
syndrome. Journal of Neurology, 223,
191-198.
- Beckmann, H., & Zimmer, R. (1981). An
ethological interpretation of stereotypy induced
by environmental stimulus. Archiveffir
Psychiatry und Nervenkrank, 230, 81-89.
- Beeson, P. B., McDermott, W., &
Wyngaarden, J. B. (Eds). (1979). Cecil textbook
of medicine (15th ed.). Philadelphia: W. B.
Saunders, Co.
- Bell, L.
A. (1980). Boredom and the yawn. Review of
Existential Psychology and Psychiatry, 17,
91-100.
- Bhangoo, K. S. (1974). Letter. New England
Journal of Medicine, 290, 1440.
- Braunwald, E., Isselbacher, K. J.,
Petersdorf, R. G., Wilson, J. D., Martin, J. B.,
& Fauci, A. S. (Eds). (1987). Harrisons
principles of internal medicine (I Ith ed). New
York: McGraw-Hill.
- Daulouede, J. P. (1980). Une nouvelle
methode de sevrage des toxicomanes par
utilisation du courant de Limoge [A new
method of eliminating drug addiction using
Limoge's current]. Annales
Medico-Psychologigues, 138, 359-370.
- De Vries, J.
1. P., Visser, G. H. A., & Prechtl, H. F.
R. (1983). The emergence of fetal behaviour:
I. Qualitative aspects. Early Human Development,
7, 301-322.
- De Vries, J.
I. P., Visser, G. H. A., & Prechtl, H. F.
R. (1985). The emergence of fetal behaviour:
II. Quantitative aspects. Early Human
Development, 12, 99-120.
- Donovan, B. T. (1978). The behavioral
actions of the hypothalamic peptides: A teview.
Psychological Medicine, 8, 305-316.
- Feldman, J. F., Brody, N., & Miller, S.
A. (1980). Sex differences in non-elicited
neonatal behaviors. Merril Palmer Quarterly, 26,
63-73.
- Flechter, S., Cohen,
F., Borenstein, F., Regev, I., & Vardi, J.
(1982). Yawning as a paroxysmal sign of
diencephalic seizures. Archives Psychology
Psychiatry Neurology, 43, 45-54.
- Fogel, A. (1980). The effect of brief
separations on 2-month-old infants. Infant
Behavioral Development, 3, 315-330.
- Friedell, A. (1974). Letter. New England
Journal of Medicine, 290, 1439-1440.
- Geschwend, J.
(1977). Yawning in a case with transecting
glioma of the pons. Fortschrift Neurologie und
Psychiatry Grenzgeb, 45, 652-655.
- Gill, N. E., White, M. A., & Anderson,
G. C. (1984). Transitional newborn infants in a
hospital nursery: From first oral cue to first
sustained cry. Nursing Research, 33,
213-217.
- Goldberg, R. L. (1983). Sustained yawning as
a side effect of imipramine. International
Journal of Psychiatry and Medicine, 13,
277-280.
- Handa, J., Nakasu, Y., & Kidooka, M.
(1983). Transient cerebral ischemia evoked
- Rollinson, R. D.,
& Gilligan, B. S. (1979). Post anoxic
action myoclonus Lance Adams Syndrome responding
to valproate. Archives of Neurology, 36,
44-45.
- Rudolph, A. M., Bamett, H. L., & Einhom,
A. H. (Eds.). (1977). Pediatrics (16th ed.). New
York: ACC.
- Sandyk,
R. (1987). Excessive yawning and progressive
supranuclear palsy. International Journal of
Neuroscience, 34, 123-124.
- Siegal, S.
(1974). Why the yawn? New England Journal of
Medicine, 290, 1027.
- Small, M. M. (1977). Covert discrimination
training: An experimental test of the assumed
functional equivalence between covert and overt
conditioning procedures. Psychological Reports,
41, 715-720.
- Suganami, S. (1977). Study on subjective
symptoms of fatigue of senior high school
students: Part 2. Study on physical load of
senior high school students. Okayama Iqakkai
Zasshi, 89, 195-218.
- Twiest, M.
(1974). Why the yawn? New England Journal of
Medicine, 290, 14391440.
TABLE 1 Yawning Etiology
Cause References
Psychological
- Boredom Bell (1980); Kishida (1973)
- Drowsiness Suganami (1977)
- Fatigue Suganami (1977)
- Separation Fogel(1980)
- Iriùtation Provine (1986)
- Autosuggestion Small (1977)
Hormonal
- Adrenocorticotropic hormone (ACTH)
Donovan(1978)
- Melanocyte-stimulating hormone (MSH)
Donovan (1978)
Neurological
- Coma and vegetative state Braunwald et
al. (1987)
- Encephalitis Beeson et al. (1979)
- Brain hypoxia Karasawa et al. (1982)
- Intracranial hypertension Beeson et al.
(1979)
- Hemiplegia Mulley (1982)
- Diencephalic epileptic seizures Fletcher
et al. (1982)
- Thalamotomy Jurko & Andy (1982)
- Fourth ventricle tumors Arai, Kita,
Komiyama, Saeki &Nagao (1986)
- Progressive supranuclear palsy Sandyk
(1987)
- Pontine tumors or lesions Bauer et al.
(1980), Geschwend (1977)
- Syncopal vertebral syndrome Ratner &
Kaisarova (1981)
Psychiatric
- Schizophrenia Beckmann & Zimmer
(1981)
- Organic psychosis Lehmann (1979)
- Involutional depression Lehmann
(1979)
- Withdrawal syndrome Daulouede (1980);
Maeda (1975); Lett et al. (1976)
General pathologic
- Increased ear cavity pressure Ase, Arai,
Iida, & Okada (1985)
- Gastric dyspepsy Braunwald et al.
(1987)
- Biliar dyskinesia Braunwald et al.
(1987)
- Car sickness in scoliotics Nakanishi et
al. (1980)
Drug overdose
- Naloxone Paroli et al. (1984);
Nemeth-Coslett
- & Griffiths (1986); O'Brien et
al.(1975)
- Valproate Rollinson & Gilligan
(1979)
- Imipramine Goldberg (1983)
- Clomipramine McLean et al. (1983)
- Seratonin Holmgren et al. (1980)
- Pentobarbital Lehmann (1979)
Drug withdrawal
- Heroin Rudolph et al. (1977)
- Morphine Rudolph et al. (1977)
- Lefétamine Paroli et al.
(1984)
- Methadone Lett et al. (1976)
- Pentazocin Maeda (1975)
  - published by HELDREF PUBLICATIONS, 4000
Albernarle Street, N.W., Washington, D.C.
20016.
- Requests for reprints should be sent to J.
J. M. Askenasy, Sleep Research Institute, Sheba
Medical Center, Tel-Hashomer 52621, Israel.
|




