- Abstract
- Yawningisastereotypicalcomplexmuscularmovementandiscommonlyexecutedbymostvertebrates.
In seconds, the entire airway is fully dilated
and surrounding muscles are powerfully
stretched, most prominently around the pharynx.
To date, yawning has been rarely studied, and as
of yet there is no consensus on its main
function.
-
- To investigate a mechanical airway function
for yawning, a literature search was conducted
to relate the frequency of yawning and
obstructive airway conditions. The results show
that changes in obstructive airway conditions
and alteration of the frequency of yawning are
temporally related.
-
- These relationships, however, cannot be
interpreted as causal, nor can they be
extrapolated to explain the function of yawning.
Yet airway management and yawning share many
physiological characteristics. We therefore
propose a novel hypotheses: yawning plays a
significant role in airway physiology by muscle
repositioning and widening the airway lumen,
thereby securing long-term oxygenation.
-
- the
video
-
- Résumé
- Le bâillement est un mouvement
musculaire complexe
stéréotypé. Il est
couramment exécuté par la plupart
des vertébrés. En quelques
secondes, les voies respiratoires sont
entièrement dilatées et les
muscles environnants sont puissamment
étirés, surtout au niveau du
pharynx. Jusqu'à présent, le
bâillement a été rarement
étudié, et il n'existe pas encore
de consensus sur sa fonction principale.
-
- Afin d'étudier la mécanique
des voies respiratoires au cours du
bâillement, une recherche documentaire a
été menée pour mettre en
relation la fréquence du bâillement
et les conditions obstructives des voies
respiratoires. Les résultats montrent que
les changements vers l'obstruction des voies
aériennes et l'altération de la
fréquence des bâillements sont
liés dans le temps.
-
- Ces relations ne peuvent cependant pas
être interprétées comme
causales, ni être extrapolées pour
expliquer la fonction du bâillement.
Pourtant, la gestion des voies aériennes
et le bâillement partagent de nombreuses
caractéristiques physiologiques. Nous
proposons donc une nouvelle hypothèse :
le bâillement joue un rôle important
dans la physiologie des voies respiratoires en
repositionnant les muscles et en
élargissant la lumière des voies
respiratoires, assurant ainsi une
oxygénation à long terme.
-
-
-
- Introduction
- General characteristics Yawning, gaping, or
oscitation is a common and stereotyped physical
behavior performed by most vertebrates,
including mammals, birds, reptiles, amphibians,
and even fish [1, 2]. In most animals, a
regular yawn lasts 4 to 7 s, and is
characterized by (1) a long inspiratory phase
with gradual mouth gaping, followed by (2) a
brief climax (or acme) with powerful muscle
stretching, and (3) a rapid expiratory phase
with muscle tension release [1, 3, 4].
For fish and birds, this is described as gradual
mouth gaping, staying open for at least 3 s and
subsequently a rapid closure of the mouth
[5]. A yawn is performed from fetal
stages to old age, in human fetuses starting
from the 11th or 12th post-conceptional week
[6, 7].
-
- Frequency of yawning
- Fetuses yawn around 25 times per day,
[8] after which the frequency decreases
with age [9]. Adults have been observed
to yawn about nine times per day (range 0-28)
[10], often in fits of two or three with
increasing intensity [3, 11]. Yawning
frequencies of animals have hardly been studied,
but convey the impression of being similar
[12, 13]. Yawning's frequency is
influenced by multiple internal and external
triggers. Primarily, a yawn is triggered in a
low-vigilance state of the brain while
transiting between wake and sleep. Both the
awaking process and progressive drowsiness
regularly provoke a yawn [1, 9, 14].
Particular stressful events (e.g., athletes
before a game), imitation of a yawn, and
hungriness have also been reported as endogenous
triggers [3, 10]. In humans and certain
social animals, yawning is sometimes triggered
by exogenous triggers: seeing or hearing another
individual yawn, or reading about yawning, which
you may have just experienced [5, 15,
16]. This is defined as contagious yawning
and can be suppressed with difficulty. Opioid
withdrawal syndrome, psychoactive drugs (e.g.,
apomorphine, naloxone after morphine), and
neurological diseases (e.g., amyotrophic lateral
sclerosis, multiple sclerosis) are related to
excessive yawning, which is defined as more than
3 yawns per 15 min [17, 18]. Opioid
peptides are known to inhibit a yawn,
[19] and some psychotic disorders may be
related to decreased yawning, of which no cutoff
value has so far been reported
[20].
-
- Basic neurology of yawning
- Yawning is a complex neuro- logical act,
mainly orchestrated in the brainstem near the
basic life centers for breathing, swallowing,
mastication, and coughing [19]. Top-down
control by cortical, limbic, and hypothalamic
centers is involved in triggering yawning and
voluntary inhibition in certain intelligent
animals [19]. A variety of neuroactive
agents have been identified to contribute to a
yawn: nitric oxide, dopamine, acetylcholine,
glutamate, serotine, adrenocorticotropic hormone
(ACTH), oxytocin, and steroid hormones
[19]. Based on lesion studies and
neuropharmacological studies, effector neurons
are thought to be the cranial nerves V, VII, IX,
X, XI, and XII (innervating the masseter,
facial, pharyngeal, laryngeal, neck, and tongue
muscles respectively), the cervical nerves
(innervating the diaphragm and scalene muscles),
and thoracic nerves (innervating the intercostal
muscles) [19, 21]. These neurons fire in
a unique rhythmical order, resulting in a
complex pattern of contracting muscles around
the respiratory and most proximal digestive
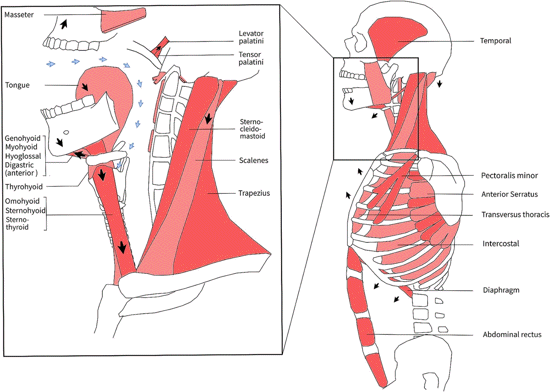
tract (anatomical overview in Fig. 1).
-
- Observe your own yawns in the mirror. If not
already triggered, one can voluntarily provoke a
yawn by inhaling gradually while retracting the
tip of the tongue and opening the jaw
repetitively.
- Fig.1 Muscle movements during a yawn:
anatomical overview. A yawn can be divided in
three phases: (1) the inspiratory phase in which
the respiratory muscles gradually contract, (2)
the climax (or acme) phase with maximal muscle
stretching, and (3) the expiratory phase with
muscle relaxation and a satisfied sensation.
During the first phase, the subhyoidal muscles
(thyrohyoid, sternohyoid, sternothyroid,
omohyoid) and floor of mouth muscles
(geniohyoid, mylohyoid, hyoglossus, and anterior
bellies of the digastric) gradually contract,
resulting in jaw opening and pharyngeal dilation
(3-4_diameter). Thereby, the diaphragm,
intercostals, and additional respiratory muscles
(e.g., scalene muscles, minor pectoral) contract
causing deep inspiration (blue arrows). Peak
forces are achieved dur- ing the second phase,
where jaw (e.g., masseter and temporal),
pharyngeal (Fig. 3), and other body muscles
(e.g., arms, trunk) are power- fully stretched
(Fig. 3). Afterwards, prolonged maximal dilation
and inspiration muscle tension are released and
expiration follows (third phase).
-
 -
- The act of yawning
- At first, gradual inspiration is caused by
contraction of the diaphragm and intercostal
muscles. Then, the mandible lowers, and the
mouth may open, defined as "gaping" (one can
yawn without opening the mouth; how- ever, this
is less satisfactory). The tip of the tongue
retracts and moves downward, accompanied by
prominent down- ward movement of the larynx and
hyoid bone, which is achieved by contracting
infrahyoidal muscles (Fig. 3) [3, 22].
Subsequently, the inspiration accelerates and
the soft palate and posto-lateral side of the
pharynx elevate, which is the point where a
turbulent inhaling sound of the palate and
clicking sounds of the opening eustachian tubes
may be experienced [23]. At this point,
the pharynx diameter has increased 3-4 times
[1, 3, 24] and the hyoid bone has
reached its nearest position to the mandible.
Peak forces of dilator muscles (agonists)
initiate the acme phase, where jaw and
pharyngeal muscles (antagonists) are maximally
stretched, often accompanied by stretching of
other body muscles (e.g., trunk, arms) [3,
25]. This is also known as the
stretch-yawning syndrome, or pandiculation (in
Latin pandare = stretching), which is primarily
observed when awakening [3]. This
powerful stretching and maximal dilation of the
airway from the mouth to alveolus takes 1 s or
less and comprises the acme phase [26].
A facial grimace, closed eyes, and sometimes
lacrimation might be observed. After the climax,
muscle tension is released and expiration
follows. This may be experienced with
vocalization and a rewarding sensation
[27]. The morphology of a yawn may,
however, depend on the (social) context
[28].
-
- Hypotheses of yawning's function
- The function of yawning's complex motor
pattern is widely debated. Four popular theories
describe the function of yawning and indicate
there is no consensus about yawning's main
function. First, the "brain arousal hypothesis"
suggests yawning diffusely activates the brain
[1]. However, brain arousal by yawning
is not evident in EEG, skin conductance, and
other autonomic parameters [29]. If
present in studies, arousal might well be
triggered by voluntary body movements
[30]. Second, the "respiration
hypothesis" describes yawning as an oxygenating
maneuver, primarily to supply the brain
[31]. This theory has been discarded
since Provine et al. (1987) could not trigger
yawning in students by exercise and by breathing
through a hand-held mask with increased CO2
levels (5%). Likewise, stimulated yawns could
not be inhibited by high (100%) O2 levels. This
study mentioned no O2 or CO2 pressures in
participants, but significant changes were not
expected by Krestel et al. (2018). Therefore, a
possible oxygenation function would not explain
(frequent) yawning in utero. This oxygenating
theory underlies the theory that a yawning
supports short-term oxygenation (or saturation),
while we suggest yawning enables ventilation by
widening the airway, which may be interpreted as
long-term oxygenation (see "Discussion"). Third,
the "communication hypothesis" is based on the
contagiousness of yawning and advocates for a
communicating or group synchronization function
[27]. Social animals only yawn
contagiously for around 10% of episodes
[14], while many other animals do not
yawn by external stimuli at all [19].
Social interaction as a main function of yawning
is not therefore supportable, though social
interaction may well co-exist as a minor
function. Fourth, the "brain cooling hypothesis"
suggests the brain temperature decreases with
yawning [32]. A recent publication of
Massen et al. (2021) supported this hypoth- esis
by relating the frequency of yawning with brain
mass [2]. However, a significant
decrease in temperature during a yawn is
physically impossible according to critical
review and calculations by physiologist Elo
[33].
-
- It is true that yawning has been studied to
a limited extent compared to other behaviors.
Due to the complex underly- ing mechanics of
yawning, the neurological and behavioral
science, and biological influences, it is
challenging to deter- mine an unambiguous
function. By conducting an anatomical and
literature study, together with inductive
(bottom-up) reasoning, we propose a new
hypothesis on the main function of yawning (see
"Discussion").
-
- Discussion
- Yawning is considered to be a primitive
behavior, as it is widely spread across the
animal kingdom, and the yawn center is located
in the vital section of the brain. An important
physiological function may explain its
evolutionary conservation.
- This scoping review supports a relationship
between (upper) airway physiology and yawning,
based on temporal relationships of yawning's
frequency change and the variation in airway
patency. According to seven included studies,
upper airway collapse during induction of
anesthesia coincides with increased yawning in a
majority of patients. However, not all patients
yawned during induction, which may be explained
by a rapid transition to deep sleep/sedation or
opiate administration. Kocaman et al.
[51] observed no yawning during propofol
induction of 51 patients. However, opioids
(remifentanil) were also administered before
observation, which is known to inhibit yawning.
Teeth clenching and opioids are related to
decreased yawning, and both conditions coincide
with OSA-like symptoms and respiratory
suppression. Whether these complications are a
direct con- sequence of decreased yawning is not
yet clear. In the study of Bartlett,
post-surgery patients were stimulated to yawn at
least 10 times per hour and were instructed to
use a spirometer, besides normal ambulation,
sigh, and other stimulations. Pulmonary
complications were significantly reduced in the
yawning group. This may suggest that pulmonary
complications result from decreased yawning, and
may potentially be prevented by stimulating
yawns. A spirometer may have been a major
confounding factor, therefore repeating the
study without spirometer could give valuable
insights.
-
- Limitations
- Yawning is one of the most rarely studied
behaviors resulting in heterogenous studies with
low level of evidence. Determinants and outcomes
of included studies were variable, which makes
identifying relationships between studies fairly
complex. Exclusion criteria were arbitrary, as
"increased" and "decreased" yawning has not yet
been defined and was therefore often based on
the subjective view of authors. Symptoms of
obstructive airway conditions varied widely and
may have different relationships with yawning,
but did not have objective parameters. Distinct
yawn patterns and intensities were not
documented. These parameters however may also
influence obstructive airway conditions, instead
of only frequency of yawning. Dilator forces
should be within the scope of future research,
as they are never or seldom described. The
temporal relationships in Table 1 should not be
interpreted as causal factors yet, as multiple
confounding factors are present and influence
both the yawning frequency and the airway
condition (e.g., low-vigilance state, thinking
of yawning, and medication). Therefore, these
relationships cannot be extrapolated to
yawning's function. Further research is
necessary to investigate the following causal
relationships: (A) decreased yawning leads to
more obstructive airway, (B) increased yawning
leads to less obstructive airway, (C) more
obstructive airway leads to increased yawning,
(D) less obstructive airway leads to decreased
yawning.
- We combine these modest results with
yawning's characteristics (see "Introduction")
to come to a novel hypothesis on the function of
yawning.
-
- Airway physiology hypothesis
- The airway physiology hypothesis entails:
Yawning secures long-term oxygenation by
creating an enlarged airway lumen by muscle
repositioning, primarily in the upper airway. A
single letter-to-the-editor by Hanning,
[52] which was found during this
literature search, mentioned this same
hypothesis; however, the mention was brief and
without discussion.
- The airway is a hollow and dynamic passage,
which must remain open at all costs. The airway
lumen is continuously subject to forces of
gravity, changing respiratory pressures, and
body movements. Therefore, the airway is largely
supported by cartilage and bony structures
(black in Fig. 2). However, similar fixation of
the airway would not be functional in the
pharynx and lungs (blue in Fig. 2). The dynamic
movements of the pharynx and lungs are
essential, and distinctively mentioned
below.
-
- Upper airway patency
- Pharyngeal muscles determine the diameter
and volume of the upper airway. These muscles
interact in a complex fashion to constrict and
dilate for different purposes: securing the
airway, swallowing, and vocalization. Upper
airway patency (or volume) is regulated by
position of the tongue, the hyoid apparatus, the
posterolateral pharyngeal walls, and the soft
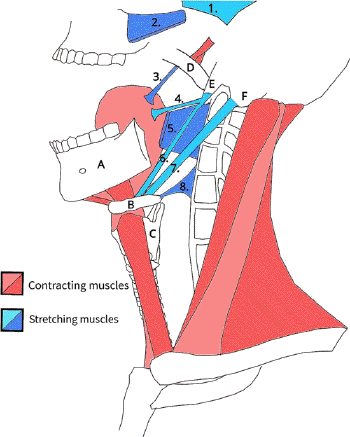
palate [53]. Muscles responsible for
these positionings are illustrated in Fig. 3 in
yawning condition. Involved muscles must be
perfectly balanced, as both loose and tight
pharyngeal
-
- In what circumstances is this muscle
repositioning and pharyngeal widening favorable?
Alteration of muscle tone throughout the body,
including pharyngeal muscles, is a result of a
changing vigilance state of the brain
[53]. Drowsiness often precedes sleep,
in which narrowing of the pharynx significantly
increases in all individuals [53]. The
upper airway is exponentially more collapsible
when the airway lumen is reduced, [53]
which is why adequate muscle tension in dilator
muscles is required during drowsiness and sleep.
Anticipatory action by dilation and muscle
repositioning is therefore essential. An example
of insufficient muscle tone during sleep is
snoring, while more serious conditions include
obstructive sleep apnea (OSA) with apneas during
the night. Most extreme are situations when the
brain is shut
- down and total collapse of the airway
follows. Unconscious patients may die due to a
collapsed pharynx, which is the reason why the
jaw thrust, chin lift, stable side position, and
intubation are life-saving
maneuvers/interventions. These widely accepted
principles underline the importance of dilator
forces in upper airway physiology. Yawning as a
key player in dilation may explain frequent
yawning around drowsiness, around sleep, during
induction of anesthesia, and excessive yawning
in patients with OSA. On the other hand, it may
also explain why decreased yawning (e.g., by
teeth clenching or opioids) coincides with
OSA-like symptoms, as was found in the results
[57, 47].
-
- Repositioning pharyngeal muscles is also
required when particular muscles have high
muscle tone after repetitive use (e.g., in
chewing, swallowing, and vocalization) or
top-down overstimulation (e.g., "lump in throat"
due to stress, emotions) [53, 58].
Already accepted is the automatic activation of
dilator muscles in the pharynx during
inspiration to prevent collapse [53]. A
compensating mechanism for variable muscle tone
due to a variable vigilance state, repetitive
swallowing, or chewing movements is not yet
described. Could yawning prevent col- lapse by
muscle repositioning in these conditions?
-
- Yawning trigger What neural feedback
mechanism may be responsible to anticipate on
airway collapse? Pharyngeal sensory feedback via
the vagal nerve was suggested by Evans (1978),
who described two cases of choking children who
yawned frequently, and stopped yawning after
obstruction was relieved. We suggest that
proprioceptive feedback from pharyngeal muscles
is essential information to orchestrate a
complex muscle balance. Proprioceptive feedback
responsible for triggering a yawn is
demonstrated by voluntarily opening the jaw
repetitively and inhaling gradually
(introduction). This imitation alters pharyngeal
muscle tones, temporarily narrows the airway,
and triggers a yawn in most individuals [3,
19, 22]. Other triggers of yawning discussed
in the "Introduction" may also result from
reduced muscle tone and accompanying
proprioceptive feedback. If extrapolated, the
beginning of a yawn might even be the trigger
for continuation of a yawn (or the "real yawn").
Relative frequent yawning of children may also
be explained by their relative narrow airway,
which makes frequent anticipation crucial.
Whether or not there is a relationship of airway
patency (indirectly implicating yawning) and
sudden infant death syndrome (SIDS) may be a
scope of future research.
-
- Yawning and atelectasis
- In the lungs, compliance is essential for
ventilation by alternate expansion and
shrinkage. This compliant property may, however,
also lead to bronchiolar and alveolar collapse
(atelectasis). This happens during sleep, when
shallow breathing and relative hypoventilation
are common due to lowered oxygen demand
[59]. Deep inspiration during a yawn, in
which lung volume increases 300-400% when
compared to tidal volume, [26] pops-open
the small airways in the lungs and secures long-
term oxygenation. This was also suggested by
Cahill et al. (1978) and Walusinski et al.
(2006). Bartlett et al. [38] stated that
yawning is functional in preventing or treating
atelectasis by prolonged maximal inflation.
Sighing and coughing are accepted maneuvers to
prevent and treat atelectasis. However, the yawn
maneuver needs further investigation to imply
such a purpose. Preventing atelectasis may also
be interpreted as a minor function of yawning,
comparable to non-verbal communication, mid-ear
pressure clearing, and other advantageous "side
effects."
-
- Fetal yawning
- Another important feature of yawning may
affect fetuses, who yawn frequently from the
first trimester to birth. Provine (2005)
proposed that fetal yawning may sculp the jaw
joint, while others stated it may help in
spreading the surfactant in utero. Some stated
it may only serve as preparation for later life
[19]. To extend our hypothesis, fetal
yawning may help airway development by
repetitive dilation and muscle repositioning.
The airway must be in perfect condition to
anticipate on one of the most critical moments
in life: the first breath.
-
- Evolutionary perspective
- Yawning is executed by almost all, if not
all vertebrates, which implies a physical
function shared by all members of this group.
One similarity is that all members have one
hollow structure used for both dilator and
constricting purposes: oxygenation by airflow or
water current versus digesting by biting,
chewing, and peristaltic movements. This is why
this hollow structure is dynamic and uniquely
modifiable by interacting muscles. These
distinct physiological functions demand opposite
muscle movements with limited fixation to the
surrounding. Oxygenation remains the top
priority, which is why strong repositioning
movements must take place to restore a vital,
dilated balance. If correct, one needs little
imagination to realize yawning has likely been
executed for millions of years, even by
dinosaurs.
-
- Future perspective
- If indeed, yawning has an important role in
airway physiology, yawning will also have
beneficial effects in patients with a
collapsible or obstructing airway. For example,
yawning may potentially counteract respiratory
complications due to opioid use (which inhibits
yawning) and OSA, and it may well influence
swallowing disorders. To sustain these
speculations, much more about yawning needs to
be studied. Suggestions for further research
include (1) imaging for precise determination of
muscles involved before, during, and after a
yawn; (2) imaging and/or flow measurements of
airway resistance and volume before and after a
yawn; (3) RCTs of the effect of stimulated yawns
on OSA, swallowing disorders, and postoperative
pulmonary
- complications (e.g., atelectasis); and (4)
animal trials of respiratory effects resulting
from absent or decreased yawning.
-
- Conclusion
- Based on the available literature and
physiological characteristics, we suggest that
yawning is the ideal maneuver to reposition all
muscles around the airway, thereby preserving
the lumen and securing long-term oxygenation.
Airway patency is therefore safeguarded by
powerful muscle stretching and dilation. This
hypothesis may explain increased yawning around
sleep, around eating, during particular
stressful events, and in children, OSA, and
other conditions with a narrowed airway.
Furthermore, yawning may be involved in fetal
airway development, and may have beneficial
effects on respiration, swallowing, and
vocalization by restoring muscle balance
[22, 60]. All these features of yawning
may help explain its evolutionary conservation,
which would make yawning one of the most
underestimated physical behaviors of modern
times.
-
- References
- 1. Baenninger R (1997) On yawning and its
functions. Psychon Bull Rev 4(2):198-207
-
- 2. Massen JJM, Hartlieb M, Martin JS et al
(2021) Brain size and neuron numbers drive
differences in yawn duration across mammals and
birds. Commun Biol 4(1):1-10
-
- 3. Barbizet J (1958) Yawning. J Neurol
Neurosurg Psychiatry 21(3):203
-
- 4. Provine RR (1986) Yawning as a
stereotyped action pattern and releasing
stimulus. Ethology 72(2):109-122
-
- 5. Baenninger R (1987) Some comparative
aspects of yawning in Betta splendens, Homo
sapiens, Panthera leo, and Papio sphinx. J Comp
Psychol 101(4):349
-
- 6. Walusinski O, Kurjak A, Andonotopo W,
Azumendi G (2005) Fetal yawning assessed by 3D
and 4D sonography. Ultrasound Rev Obstet Gynecol
5(3):210-217
-
- 7. De Vries JIP, Visser GHA, Prechtl HFR
(1985) The emergence of fetal behaviour. II.
Quantitative aspects. Early Hum Dev
12(2):99-120
-
- 8. Giganti F, Hayes MJ, Cioni G, Salzarulo P
(2007) Yawning frequency and distribution in
preterm and near term infants assessed
throughout 24-h recordings. Infant Behav Dev
30(4):641-647
-
- 9. Zilli I, Giganti F, Uga V (2008) Yawning
and subjective sleepiness in the elderly. J
Sleep Res 17(3):303-308
-
- 10. Baenninger R, Binkley S, Baenninger M
(1996) Field observations of yawning and
activity in humans. Physiol Behav
59(3):421-425
-
- 11. Szechtman H (1984) Timing of yawns
induced by a small dose of apomorphine and its
alteration by naloxone. Prog Neuro-
Psychopharmacology Biol Psychiatry
8(4-6):743-746
-
- 12. Troisi A, Aureli F, Schino G, Rinaldi F,
de Angelis N (1990) The influence of age, sex,
and rank on yawning behavior in two species of
macaques (Macaca fascicularis and M. fuscata).
Ethology. 86(4):303-310
-
- 13. Rasa OAE (1971) The causal factors and
function of yawning in Microspathodon chrysurus
(Pisces: Pomacentridae). Behaviour
39(1):39-57
-
- 14. Deputte BL (1994) Ethological study of
yawning in primates. I. Quantitative analysis
and study of causation in two species of Old
World monkeys (Cercocebus albigena and Macaca
fas- cicularis). Ethology 98(3-4):221-245
-
- 15. Platek SM, Mohamed FB, Gallup GG Jr
(2005) Contagious yawning and the brain. Cogn
brain Res 23(2-3):448-452
-
- 16. Provine RR (2005) Yawning: the yawn is
primal, unstoppable and contagious, revealing
the evolutionary and neural basis of empathy and
unconscious behavior. Am Sci 93(6):532-539
-
- 17. Krestel H, Weisstanner C, Hess CW,
Bassetti CL, Nirkko A, Wiest R (2015) Insular
and caudate lesions release abnormal yawning in
stroke patients. Brain Struct Funct
220(2):803-812
-
- 18. Erkoyun HU, Beckmann Y, Bülbül
NG, I_ncesu TK, Kanat NG, Ertekin C (2017)
Spontaneous yawning in patients with multiple
sclerosis: a polygraphic study. Mult Scler Relat
Disord 17:179-183
-
- 19. Krestel H, Bassetti CL, Walusinski O
(2018) Yawning, its anatomy, chemistry, role,
and pathological considerations. Prog Neurobiol
161:61-78
-
- 20. Lehmann HE (1979) Yawning: a homeostatic
reflex and its psychological significance. Bull
Menninger Clin 43(2):123
-
- 21. Walusinski O, Neau J-P, Bogousslavsky J
(2010) Hand up! Yawn and raise your arm. Int J
Stroke 5(1):21-27
-
- 22. Boone DR, McFarlane SC (1993) A critical
view of the yawn-sigh as a voice therapy
technique. J Voice 7(1):75-80
-
- 23. Laskiewicz A (1953) Yawning with regard
to the respiratory organs and the ear. Acta
Otolaryngol 43(2-3):267-270
-
- 24. Walusinski O (2006) Yawning: unsuspected
avenue for a better understanding of arousal and
interoception. Med Hypotheses 67(1):6-14
-
- 25. Bertolucci LF (2011) Pandiculation:
nature's way of maintaining the functional
integrity of the myofascial system? J Bodyw Mov
Ther 15(3):268-280
-
- 26. Corey TP, Shoup-Knox ML, Gordis EB,
Gallup GG Jr (2012) Changes in physiology
before, during, and after yawning. Front Evol
Neurosci 3:7
-
- 27. Daquin G, Micallef J, Blin O (2001)
Yawning. Sleep Med Rev 5(4):299-312
-
- 28. Zannella A, Stanyon R, Maglieri V,
Palagi E (2021) Not all yawns tell the same
story: the case of Tonkean macaques. Am J
Primatol. Published online :e23263
-
- 29. Guggisberg AG, Mathis J, Schnider A,
Hess CW (2010) Why do we yawn? Neurosci Biobehav
Rev 34(8):1267-1276
-
- 30. Guggisberg AG, Mathis J, Herrmann US,
Hess CW (2007) The functional relationship
between yawning and vigilance. Behav Brain Res
179(1):159-166
-
- 31. Gorter D (1755) De Perspiratione
Insensibili
-
- 32. Gallup AC, Gallup GG Jr (2008) Yawning
and thermoregulation. Physiol Behav
95(1-2):10-16
-
- 33. Elo H (2010) Yawning and
thermoregulation. Sleep Breath 14(4):391
-
- 34. ProQuest Refworks 2.0, Ann Arbor,
Michigan, USA. Published online 2008
-
- 35. Schoot R van de. © ASReview
(2019-2021): Active learning for systematic
reviews. https://asreview.nl/
-
- 36. Cincinnati Children's Hospital Medical
Center. LEGEND table of evidence. Published
2012. Accessed 12 Jan 2020. https://www.
cincinnatichildrens.org/research/divisions/j/anderson-center/evide
nce-based-care/legend
-
- 37. Grant MJ, Booth A (2009) A typology of
reviews: an analysis of 14 review types and
associated methodologies. Heal Inf Libr J
26(2):91-108
-
- 38. Bartlett RH, Gazzaniga AB, Geraghty T
(1971) The yawn maneuver: prevention and
treatment of postoperative pulmonary
complications. In: Surgical Forum 22:196
-
- 39. Evans E B (1978) Yawning in pharyngeal
obstruction. BMJ 1(6110):443-444.
https://doi.org/10.1136/bmj.1.6110.443-c
-
- 40. Mukai S, Mukai C, Asaoka K (1991).
Ankyloglossia with deviation of the epiglottis
and larynx. Ann. Otol. Rhinol. Laryngol
100(5_suppl), 3-20
-
- 41. Kim DW, Kil HY, White PF (2002)
Relationship between clinical endpoints for
induction of anesthesia and bispectral index and
effect-site concentration values. J Clin Anesth
14(4):241-245
-
- 42. Kasuya Y, Murakami T, Oshima T, Dohi S
(2005) Does yawning represent a transient
arousal-shift during intravenous induction of
general anesthesia? Anesth Analg
101(2):382-384
-
- 43. Oshima T, Utsunomiya H, Kasuya Y,
Sugimoto J, Maruyama K, Dohi S (2007)
Identification of independent predictors for
intra-venous thiopental-induced yawning. J
Anesth 21(2):131-135.
- https://doi.org/10.1007/s00540-006-0490-x
-
- 44. Tsou C-H, Kao T, Fan K-T, Wang J-H, Luk
H-N, Koenig HM (2008) Clinical assessment of
propofol-induced yawning with heart rate
variability: a pilot study. J Clin Anesth
20(1):25-29
-
- 45. Oshima Tsutomu, Murakami Tatsuo, Saitoh
Yuhji, Yokota Miyuki, Kasuya Yoshiko (2010)
Inhibitory effects of landiolol and nicardipine
on thiopental-induced yawning in humans. J
Anesth 24(2):168-172.
https://doi.org/10.1007/s00540-010-0879-4
-
- 46. Gallup GG, Gallup AC (2010) Excessive
yawning and thermoregulation: two case histories
of chronic, debilitating bouts of yawn- ing.
Sleep and Breathing 14(2):157-159
-
-
-
- 47. Carra MC, Huynh N, Morton P et al (2011)
Prevalence and risk factors of sleep bruxism and
wake-time tooth clenching in a 7-to 17-yr-old
population. Eur J Oral Sci 119(5):386-394
-
- 48. Tsou C-H, Yu P-Y, Tu P-Y, Fan K-T, Luk
H-N, Kao T (2012) Altered short-term dynamics of
cardio-respiratory interaction during
propofol-induced yawning. Chin J Physiol
55(3):169-177
-
- 49. Zaharna M, Rama A, Chan R, Kushida C
(2013) A case of positional central sleep apnea.
J Clin Sleep Med 9(3):265-268
-
- 50. Catli T, Acar M, Hanci D, Arikan OK,
Cingi C (2015) Importance of yawning in the
evaluation of excessive daytime sleepiness: a
prospective clinical study. European Archives of
Oto-Rhino-Laryngology 272(12):3611-3615
-
- 51. Kocaman Akbay B, Demiraran Y, Yalcin
Sezen G, Akcali G, Somunkiran A (2007) Use of
the bispectral index to predict a positive
awareness reaction to laryngeal mask airway-
Fastrach insertion and intubation. Acta
Anaesthesiol Scand 51(10):1368-1372
-
- 52. Hanning CD (2001) Yawning. Sleep Med Rev
5(5):411
-
- 53. Ayappa I, Rapoport DM (2003) The upper
airway in sleep: physiology of the pharynx.
Sleep Med Rev 7(1):9-33
-
- 54. Reed WR, Roberts JL, Thach BT (1985)
Factors influencing regional patency and
configuration of the human infant upper airway.
J Appl Physiol 58(2):635-644
-
- 55. Taylor DC, Dalton JRJD, Seaber AV,
Garrett JRWE (1990) Viscoelastic properties of
muscle-tendon units: the biomechanical effects
of stretching. Am J Sports Med
18(3):300-309
-
- 56. Titze IR, Bergan CC, Hunter EJ, Story B
(2003) Source and filter adjustments affecting
the perception of the vocal qualities twang and
yawn. Logop Phoniatr Vocology 28(4):147-155
-
- 57. Van Ryswyk E, Antic NA (2016) Opioids
and sleep-disordered breathing. Chest
150(4):934-944
-
- 58. Akin M, Kurt MB, Sezgin N, Bayram M
(2008) Estimating vigilance level by using EEG
and EMG signals. Neural Comput Appl
17(3):227-236
-
- 59. Douglas NJ, White DP, Pickett CK, Weil
JV, Zwillich CW (1982) Respiration during sleep
in normal man. Thorax 37(11):840-844 60. Xu JH,
Ikeda Y, Komiyama S (1991) Bio-feedback and the
yawn- ing breath pattern in voice therapy: a
clinical trial. Auris Nasus Larynx
18(1):67-77
-
|




