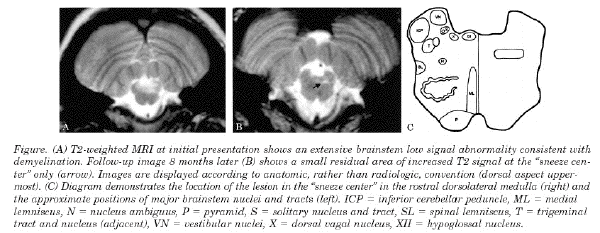
To the Editor: Experiments in cats
identified a concentration of cells in the
rostral dorsolateral pontomedullary area,
stimulation of which causes sneezing
indistinguishable from sneezing induced by
natural peripheral stimuli. The effect of
ablation of these cells has not been studied,
but in humans one case with a medullary tumor
and four cases with lateral medullary syndrome
have been described with abortive sneeze reflex
(ASR). The inspiratory phase was not followed by
the explosive expiratory phase in these
individuals, although it could voluntarily be
reproduced. All five cases experienced complete
recovery of the sneeze reflex within months. The
most recent description of a patient with
systemic lupus erythmatosus-related
demyelination who had ASR with a persisting
lesion in the area of sneeze centerl is further
evidence that ASR results from a well-defined
brainstem lesion.
The subject may, however, be more complex, as
the following case illustrates. The patient was
a 79-year-old man with sudden onset of right
facial weakness and right hemiparesis.
Subsequently, he became obtunded and
disoriented; his speech output consisted of
words, but was inappropriate most of the time.
CT scanning showed hernorrhage in the area of
left basal ganglia. He improved during the next
few days only to deteriorate again into a
semivegetative state. During the days he showed
improvement, his wife and daughter observed four
episodes within an hour that were typical for
ASR. In this patient there was no evidence for
involvement of the brainstem either clinically
or on the CT scan. The fact that patients with
ASR can mimic the expiratory phase of sneezing
and that it can be voluntarily suppressed in
healthy individuals suggests a cortical
influence on the sneezing mechanism. It is pure
speculation whether interruption of the
corticobulbar connections caused ASR in this
patient. The important point is that ASR can
occur in the absence of a lesion in the sneeze
center in the brainstem.
The patient's wife made the interesting
comment: "I thought it was normal" So had I
until I read Dr. Hersch's report. I have
experienced ASR many times and have observed it
in family members, friends, and patients. Normal
ASR tends ta be sporadic and occurs in the
middle of a series of completed sneezes. It is
most likely the result of subthreshold.
recruitment in the neurons in the pontomedullary
sneeze center.
Beyond the scientific value, observations
like A.SR serve the purpose of helping
clinicians localize abnormalities. Because ASR
can be normal or pathologic and the pathologie
can be due to a brainstem and or a hemispheric
lesion, a more firm statistical connection
between ASR and brain lesions has to be
established before it can be used for
localization purposes. A stroke clinic or an MS
center may be the best place ta study and
establish such connection. Leslie Suranyi, MD,
FRCP(C), Cornwall, Ontario, Canada
Reply from the Authors: I thank Dr.
Suranyi for his interest in my report. He
correctly points out that the sneeze reflex can
be influenced by brain regions above the
medulla. The cortical influence on sneezing is
recognized by most individuals who can at least
partially suppress the reflex voluntarily. In
addition, the photic sneeze response is well
described and a circadian influence on sneezing
has also been suggested.
However, it is difficult to interpret the
signs related to Dr. Suranyi by relatives of his
patient, who, evidently, was not able to report
his own experience. It is possible that the
observed sudden inspirations were due to
yawning, for example. Even if abortive
sneezing is assumed, the observation of several
episodes within an hour without obvious external
triggers for sneezing might suggest that the
basal ganglia hemorrhage resulted in stimulation
of the input side of the sneeze reflex, without
the threshold for sneeze generation being
met.
By contrast, my patient and the previously
described patients with medullary lesions all
reported the occasional urge ta sneeze in
response to normal stimulation and sensation,
but were unable to "enjoy" a completed sneeze.
These patients were able ta mimic a sneeze
voluntarily, however, indicating that despite
both input and output comportents of the sneeze
reflex being preserved, the sneeze reflex was
interrupted by the medullary lesion.
Although Dr. Suranyi's experience indicates
that the outward signs suggestive of abortive
sneezing might not be specific to lesions in the
medulla, the evidence currently available
continues to support the model of an integrative
sneeze center in the dorsolateral medulla.The
sneeze center receives input from sources
including the first and second divisions of the
trigeminal nerve and higher centers, and
triggers a specific, coordinated, all-or nothing
motor response when a critical threshold is
exceeded. Interaction between the centers on
each side must be postulate to explain that the
inability to sneeze may result from unilateral
lesions involving the sneeze center. From a
clinical point of view it is important to note
that all of the reported patients with a los of
the ability ta sneeze due to a medullary lesion
also had othe signs of a brainstern disorder at
their first presentation