Yawning
and stroke
The locked-in syndrome (LIS) denotes a
neurological condition due to bilateral
transsection of pyramidal tracts at the level of
pons or cerebral peduncles leading to complete
immobility, except for vertical gaze. The
syndrome shows several varieties in terms of the
symptoms and course, the subject of a previous
paper .
In locked-in patients a number of movements
had been observed that were incompatible with
the extent of voluntary paralysis. Since the LIS
represents a unique natural transsection
experiment with preserved consciousness, the
investigation of those motor phenomena promised
some insight in the organization and
localization of nonpyramidal motor systems. The
present paper gives a description and list of
these movements and outlines the possible
explanations.
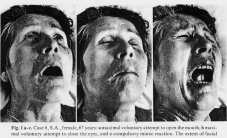
Case 6. S.A., a woman aged 67. During
the acute phase of the nearly classical LiS
groaning was noted. It occurred spontaneously
and also secondary to attempted verbal
communication. Seven days after admission,
yawning accompanied by typical
generalized body stretching was noted. The
observation was made while recording an EEG. The
tracing was judged within normal limits, and
cerebral electrical activity remained unchanged
during the yawning. The patient's condition
improved to an incomplete LIS. Ocular motility
became free. some crude sounds could be uttered
voluntarliv, and quadriplegla was also slightly
improved. During this phase the patient
exhibited compulsory munic reactions by far
exceeding the extent of motions already possible
by voluntary innervation. Those compulsory mimic
reactions were frequently, but not invariably,
accompanied by a penetratingly loud crying.
Urging the patient to stop was never successful,
and it never became clear whether the crying was
secondary to external or internal distress. The
next month crying was frequently repeated each
day. The repetition seemed to follow an
endogenous pattern linked with the well
developed steep cycles. There were hours of
regular crying at a rate of once or twice a
minute. In clinical jargon we coined the terrn
"cat crying" for this rather trouble some
symptom. When paralysis of cranial nerve muscles
further improved cat crying and eventually
compulsory mimic reactions disappeared.
Discussion
Normal motor functions are the result of an
interaction of sensory input, of processing by
integrative cortical areas, and of programing by
the primary motor cortex. This program is
carried out with the support of the
extrapyramidal system, of the cerebellum, or
primordial motor patterns built-in at different
levels of the brain stem, and of reflexes
mediated by the spinal cord. Under pathological
conditions abnormal involuntary motor phenomena
appear or normal movements occur in an
uncontrolled autornatic fashion. The studies of
those motor phenomena have brought remarkable
insights in the organization of the motor
svstem, occasionally marred by somewhat
whimsical speculations about the biological goal
of these patterns. However, motor phenomena
might be divided into normal reactions, complex
automatic behavior, and simple reflexes.
Normal reactions are variable and represent
appropriate responses to the changing demands of
the environment. Automatic motor patterns such
as motorische Schablonen or motorische
Primitivschablonen appear in a stereotyped
fashion and are considered primordial behavior
organized somewhere in the subcortical
structures and released under pathological
conditions by the lacking influence of cortical
inhibiting systems. Therefore, automatic motor
patterns have been observed in coma, in chronic
vegetative state or apallic syndrome, in cases
of bilateral supranuclear palsy [34], in
cerebral malformations, and in normal inborns.
The examination of' motor phenomena in high
pyramidal transsections like the LIS can be of
great value to disclose the localization of the
so-called centers of such motor patterns. In
LIS, it seems to be easy to differentiate
involuntary motor phenomena from remnants of
pyramidal movements. The conscious patients use
the later ones for communication. However, most
of the pathological patterns are
stimulussensitive, and it might be hard to
decide in a particular case, whether the move
ments are secondary to. command or to
nonspecific stimulation. Repeated examination
and the consideration of the unvariable type of
the pathological motor pattern may lead to the
proper diagnosis.
Extensor spasms (decerebrate
posturing) were frequently seen with the LIS
(Table 1) and were in.variably
stimulus-sensitive. Neck deflection was
especially effective (case 2). Extensor spasms
are identical with Jackson's cerebellar fits and
are a constitutional sign of midbrain affection
due to transtentorial hernation or functional
dissolution down to the midbrain level due to
metabolic or anoxic encephalopathies. Gamper
showed both extensor and flexor spasms in the
ancephalic midbrain. Since extensor spasms were
also seen in localized brain stem lesions with
intact cortical functions, the term decerebrate
posturing is intrinsically fallacious. This
statement is strongly supported by the
observations in LIS. Extensor spasms disappear
with dissolution of bulbar brain functions.
These clinical observations suggest that
extensor spasms are stimulus-sensitive-composed
reflexes built-in within the bulbar brain and
released by interruption of inhibiting pyramidal
influences somewhere above the midbrain level.
These limits were already established by the
experimental work of Sherrington.The closer
localization lies within the multisynaptic
system of the brain stem intimately related to
the ascending reticular activating system . A
connection of the stretch reflex with a diffuse
activating system in the brain stem was aiready
suspected as early as 1926 by Gamper.
Flexor spasm (decorticate posturing)
was rarely observed in LIS. Case 4 was an
incomplete LIS with motor remnants of all four
extremities. From the observations in
transtentorial herniations one has to draw the
conclusion that flexor spasms are integrated
above the midbrain-diencephalic border. This
might be the reason why it is exceptionally
observed in LIS and only in the incomplete
form.
Pain reactions, compulsory mimic
reactions (Zwangsweinen) and compulsory
screaming (cat crying) have been separately
listed in Table 1, although these patterns
cannot be distinguished by the mere description
of the motor phenomenon. The pain reaction
represents a normal phenomenon secondary to
specific stimulation, abolished with certain
depressed cerebral states and exaggerated with
others. Compulsory mimic reactions occur with
nonspecific stimulation and are frequently
repeated. The differentiation from an
exaggerated pain reaction may be impossible and
meaningless in a practical as well as in a
theoretical sense. Cat crying occurs
spontaneously in an automatic repetition rate
with an extremely pronounced vocal component. In
LIS, pain reactions were seen in four cases of
the presented series during the acute phase but
were reported in literature only once. Its
facial and vocal components are integrated in
the periaqueductal gray. Its occurrence in LIS
suggests that the pathways to the corresponding
cranial nerve nuclei do not use the pyramidal
tracts interrupted in LIS but instead a
primordial motor system within the dorsal part
of the brain stem.
There are several observations of compulsory
mimic reactions (Zwangsweinen) in chronified
LiS. It occurs spontaneously and in a rhythmic
pattern like other cases of severe supranuclear
palsy . Pathological crying is organized in the
brain stem and usually appears in conjunction
with bilateral pyramidal or extrapyramidal motor
disorders . Laughing was never observed in LIS.
Therefore, it has to be integrated in the rostal
brain stem above the lesions leading to a LIS.
This is in line with the findings in
malformations. Cat crying may be separated from
the vocal component of the pain or compulsory
mimic reactions. It is crude and shrill like the
screaming of prematures. Neumann described
spontaneous and automatic screaming in children
with tumors in the rostral brain stem.
Sherrington and Catel and Krauspe suppose a
primordial system for vocalization in the oral
brain stem whose irritation or disinhibition
might also be responsible for cat crying in
LIS.
Yawning was also seen in LIS.
Observations in the apallic syndrome, in
cerebral malformations, in inborns and
prematures, and in the early phases of
transtentorial herniations make it likely that
it is integrated in the lower brain stem, an
area undisturbed by ventral pontine syndromes.
Yawning also contains generalized body
stretching resembling extensor spasms, and the
whole sequence of behavior is finished by
swallowing.Conncections with the sleep-inducing
system, the arousal system, or the respiration
center were conjectured.
The REM sleep and to a lesser degree, the
NREM sleep is altered in LIS. The changed sleep
pattern is not due to immobility such as that in
high cervical lesions but to the direct
involvement of the sleep-inducing system within
the brain stem. REM sleep reduction was only
seen with paralyzed horizontal gaze, whereas
incomplete LIS with preserved lateral eye
movements had comperatively undisturbed sleep
cycles . These findings prompted the assumption
that the paramedian pontine reticular formation
known to be responsible for conjugate gaze
movements at the pontine level might also be
related to induction or priming the REM sleep.
However, the relation of the sleep system to
yawning remains unclarified.
Breathing is certainly affected in LIS. The
pattern may be very regular (cases 1 and 3)
resembling the central neurogenic
hyperventilation or even ataxic (cases 4 and 5).
Peiper considered the nervous structures for
yawning to be part of the respiratory center,
suppressed under normal circumstances, but
activated or released with disturbed breathing.
This conjecture cannot be confirmed or rejected
by the findings in LIS.
Further motor phenomena like whining,
moaning, groaning, chewing, and coughing were
incidentally observed in LIS. With those
phenomena, the differentiation to residues of
voluntary motions is particularly difficult
except for coughing which appeared clearly
reflexlike to tracheal suction. Chewing or other
oral automatisms were never seen in the cases
reported and only once in the literature. In
contrast, oral motor patterns reappear tirst in
apallic patients and were fully developed in
cerebral malformations. This contrast indicates
an important difference between primary or
prolonged and acute decerebrate or cerebrobulbar
disconnection syndromes.